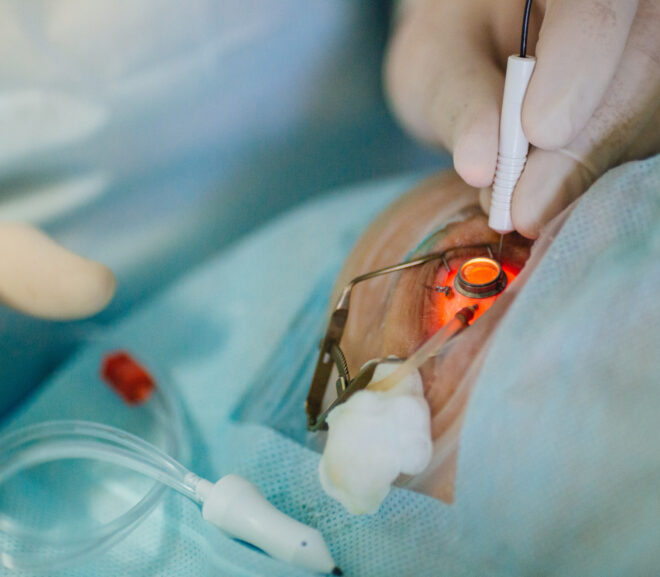
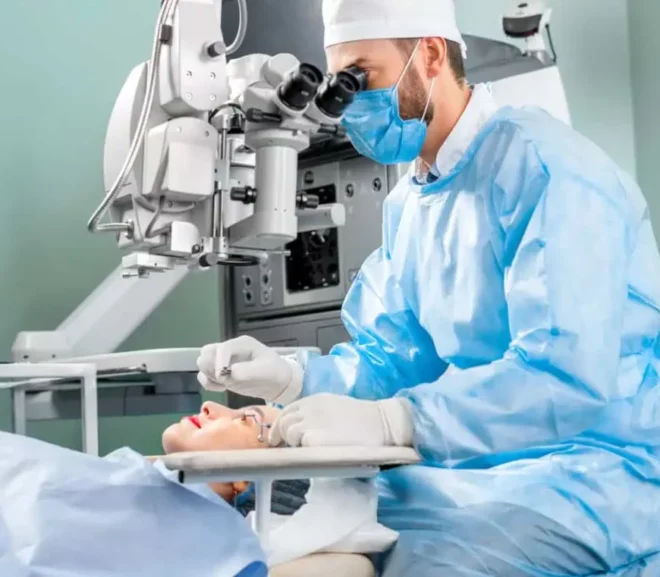
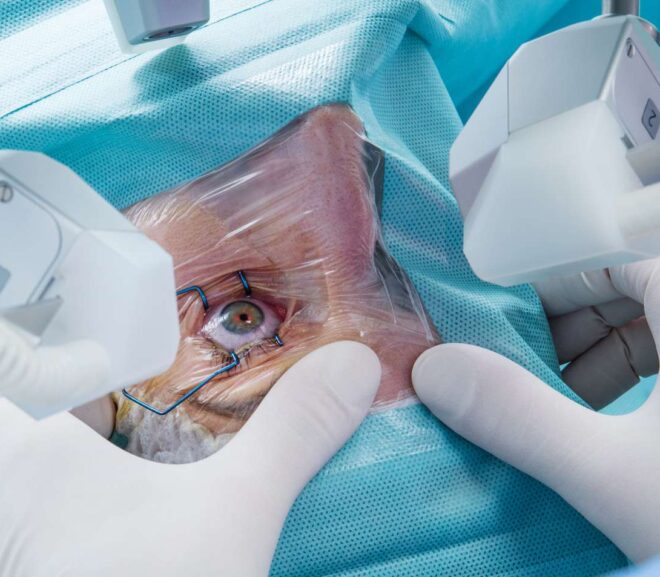
Introduction If you’ve ever imagined waking up and seeing clearly without reaching for glasses or contact lenses, you’re not alone. LASIK eye surgery has helped…
Introduction Imagine waking up and seeing the world clearly — without reaching for glasses or contact lenses. That’s the reality for millions who have undergone…
Sleep is a vital component of overall health and well-being, yet many individuals struggle with sleep disorders, particularly obstructive sleep apnoea (OSA). Continuous Positive Airway…
Sleep apnea is a serious sleep disorder that affects millions of individuals worldwide. Characterised by repeated interruptions in breathing during sleep, it can lead to…
Sleep disorders are increasingly recognised as significant health issues, affecting millions of Australians. In Sydney, the demand for sleep tests has surged as more people…
In recent years, the understanding of sleep disorders has evolved significantly, leading to innovative solutions that cater to the needs of patients. One such advancement…
Cataracts are a common visual impairment that many people experience as they age. While they are often treatable, understanding when to seek intervention can be…
Cataract surgery is a common procedure that can significantly enhance an individual’s quality of life by restoring clear vision. For residents of Sydney, understanding the…
In the world of sleep apnea treatment, ResMed has been a trusted name for over 30 years. The ResMed AirSense 10 is a powerful, reliable,…
The use of any kind of treatment has become much simpler and more widespread as a result of scientific developments in the medical fields. It…